Cause of jaundice
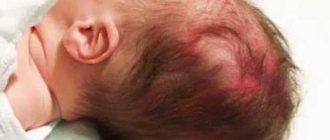
Let's look at what causes jaundice in newborns. The yellow color results from the breakdown in the newborn’s body of a substance that replaces hemoglobin in the blood. During the breakdown process, bilirubin is formed. If the baby's liver does not cope with the removal of bilirubin quickly, then a yellow color appears. This is the main reason why a newborn baby turns yellow.
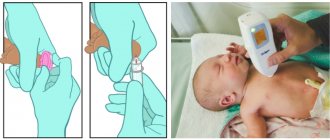
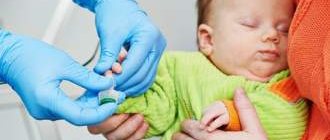
The amount of bilirubin is determined by a special blood test. It is usually taken from the heel into a special tube.
What causes jaundice?
Jaundice occurs when there is too much bilirubin in the blood.
It can be elevated due to many factors: abnormalities in the liver, impaired flow of bile (bile itself contains bilirubin) from the gallbladder and bile ducts, blood disorders in which too many red blood cells containing bilirubin are broken down. Bilirubin is a yellow substance produced by the breakdown of red blood cells that carry oxygen throughout the body. When red blood cells die, the liver filters their breakdown products from the bloodstream. But with pathologies (diseases of the liver and bile ducts, increased destruction of red blood cells), the liver may not keep up with this process, bilirubin accumulates, and the skin, sclera of the eyes and mucous membranes become yellow.
Types of jaundice
Physiological jaundice
Physiological jaundice in newborns, also known as neonatal jaundice, occurs 2-3 days after birth and disappears completely after a maximum of two weeks. It proceeds without complications and has no symptoms other than yellow color. Most doctors consider it not a disease, but a condition that occurs when the newborn body adapts to a new environment.
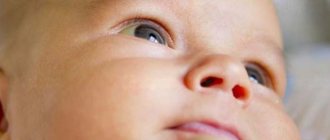
Symptoms of physiological jaundice are yellow color of the skin, whites of the eyes, and mucous membranes.
It proceeds easily and without complications.
Photo source: shutterstock.com
Types of physiological jaundice:
- jaundice of premature babies;
- hereditary;
- breastfeeding jaundice;
- jaundice due to asphyxia;
- medicinal jaundice.
Causes of physiological jaundice:
- hemoglobin breakdown;
- immaturity of internal organs (liver and spleen);
- the child was born premature;
- lack of breast milk;
- weight loss of the newborn.
Pathological jaundice
Pathological jaundice in newborns occurs earlier or later than physiological jaundice and lasts more than two weeks. It occurs much less frequently than physiological symptoms and requires hospital treatment.
Symptom:
- the appearance of a greenish tint in the yellowness of the skin and eyes;
- enlarged liver and spleen;
- stool becomes light, discolored;
- urine darkens;
- general deterioration in the health of the newborn;
- lethargy and drowsiness of the baby;
- the child sucks sluggishly or refuses to eat at all;
- the appearance of bruises on the skin for no reason.
Causes of pathological jaundice:
- incompatibility of the Rh factor of the blood of mother and baby;
- diseases of the biliary tract;
- liver infection;
- deviations in the development of the circulatory system;
- heredity;
- birth injury;
- diabetes mellitus in the mother.
In addition, there are several types of pathological jaundice.
Hemolytic jaundice
Occurs in no more than 1% of newborns.
Symptoms:
- yellowing of the skin and eyeballs 1-2 days after birth;
- enlarged liver and spleen;
- lethargy of the baby.
The reason is a discrepancy between the Rh factor of the blood of the mother and child.
Treatment must be started urgently, since the hemolytic form can become nuclear.
Kernicterus
Jaundice is called so because during its development, cell nuclei are damaged. This is one of the most dangerous varieties, as it entails serious consequences.
Symptoms:
- muscle hypertonicity and cramps;
- a sharp deterioration in the general condition of the child;
- sudden tilting of the newborn's head back.
Causes:
- conflict between the Rh factor of mother and child;
- birth injuries;
- lack of vitamin K;
- use of certain medications by the mother during pregnancy;
- fetal hypoxia;
- genetic predisposition;
- metabolic disease;
- underdevelopment of internal organs.
Obstructive jaundice
Occurs when the bile ducts are blocked. For example, compression of the duct. It is most often treated with surgery.
Reasons for appearance
If physiological causes in most cases are not a cause for concern, and the symptoms of jaundice go away on their own, then pathological ones require systematic examination and quite a long treatment.
Physiological reasons
For what reasons does the level of bilirubin in the blood remain stably high for 3-21 days?
- An increased process of fetal hemoglobin breakdown after the birth of a child, when a completely healthy liver does not have time to break down bilirubin.
- My mother was diagnosed with diabetes. The breakdown of the yellow substance in the child’s body is slowed down.
- Increased production of estrogens - female hormones that enter the baby's body with breast milk and disrupt the processing of bilirubin.
- Break from breastfeeding. If for some reason a newborn does not receive mother's milk in the first days of life, then the excretion of meconium (original feces) slows down. This can cause jaundice.
Mom should be wary if the skin, mucous membranes and eye sclera, in addition to “lemon” and “orange”, also acquire a green tint.
Pathological causes
If after 21 days positive dynamics do not appear and the child continues to “turn yellow,” it is urgent to figure out why liver enzymes do not fully break down bilirubin. Analyzes and tests make it possible to determine in which link of the “chain” the failure occurs. The health and life of the child may be under serious threat. In rare cases, there are deaths.
The reasons may be the following:
- Differences in blood type and Rh factor between mother and child. This type of jaundice is called hemolytic.
- The child suffers from congenital liver pathologies (for example, hereditary hepatitis). Bilirubin is not processed enough. The type of disease in this case is called conjugation.
- The organ is affected by a pathogenic virus (concomitant infectious disease). This is hepatic jaundice.
- Diseases of the gallbladder (may be accompanied by obstruction of the bile ducts, and therefore a disruption in the production of enzymes). In this case, the symptom is called mechanical.
If jaundice is caused by physiological reasons, the child feels fine. Pathological conditions are accompanied by a number of unpleasant symptoms.
Depending on the causes, the following symptoms occur:
Treatment
Attention. Treatment of jaundice in children should be prescribed by a doctor and carried out under his supervision. All types of pathological jaundice are treated only in a hospital.
For physiological jaundice, no specific treatment is required. To help your child cope with the excretion of bilirubin, you need to:
- put the baby to the breast as often as possible;
- refuse artificial mixtures;
- spend more time in the fresh air;
- give the baby air and sun baths;
- a nursing mother should adhere to a strict diet, excluding foods that negatively affect the gastrointestinal tract.
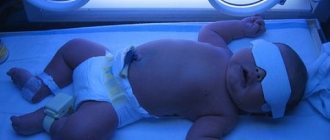
Phototherapy also has a positive physiotherapeutic effect on infantile jaundice. The essence of the method is the therapeutic effect of ultraviolet rays, which convert bilirubin in the child’s blood into a safe isomer that is easily excreted in urine and feces.
For this, a special lamp is used, under which the baby is placed for several days from 2 to 96 hours with breaks for feeding. The procedure must be prescribed by a doctor and carried out under the supervision of specialists. Phototherapy treatment is not prescribed for severe conditions and high bilirubin levels.
Photo source: shutterstock.com
Drug therapy is also carried out in the hospital as prescribed by a doctor. The child may be prescribed intravenous solutions of potassium, magnesium, and glucose. Sorbents are prescribed (Polysorb, Smecta). In severe conditions, blood transfusions are prescribed.
Treatment of jaundice in newborns
With the physiological variant, there is no need for therapy. The defect goes away on its own as the bilirubin level stabilizes. Therapeutic measures include creating conditions for a speedy recovery.
This is interesting: Obstructive jaundice in newborns: what is it, causes, treatment and consequences
After discharge from the maternity hospital, it is recommended to often walk with the child outdoors. The yellowness of the skin in babies goes away thanks to short-term sunbathing in the warm season. Breastfeeding promotes proper liver function.
During lactation, the mother is recommended to follow a gentle diet. Foods that overload the liver and digestive organs are excluded from the diet.
The pathological form is treated taking into account the cause of its occurrence. Therapy is carried out on an inpatient basis. Various methods are used: drug therapy, physiotherapeutic procedures, surgical interventions.
Consequences of neonatal jaundice
Why is jaundice dangerous in newborns? The consequences of jaundice depend on the severity of its course and the timeliness of treatment. Physiological usually has no consequences. But if pathological jaundice develops and treatment is delayed, the consequences can be extremely severe:
- lethargy;
- mental underdevelopment;
- brain damage;
- mental retardation;
- partial or complete immobility;
- cerebral palsy;
- partial blindness and deafness (with severely advanced disease);
- encephalopathy.
In particularly severe cases, swelling of the brain occurs, which can lead to the death of the child.
It is important to see a doctor in time and start treatment.
Symptoms of jaundice
From the name of the syndrome it is clear what the main symptom is.
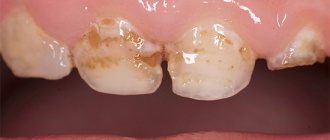
With jaundice, the whites of the eyes, skin and other tissues of the human body turn yellow. Interestingly, the shade of yellow suggests the type of jaundice. With hemolytic jaundice, the skin becomes pale and acquires a light yellow, lemon tint. For liver diseases - orange. With mechanical jaundice, the skin darkens and becomes earthy, greenish in color. Jaundice caused by acute illness is usually accompanied by fever, chills, abdominal pain, flu-like symptoms, dark urine, and light-colored stools.
If jaundice develops as a result of chronic pathology, there may be symptoms such as weight loss or itchy skin. Jaundice caused by cancer of the pancreas or biliary tract may be accompanied by abdominal pain.
Gilbert's syndrome
Separately, it is worth highlighting Gilbert's syndrome - a common hereditary disease, also known as constitutional liver dysfunction and familial non-hemolytic jaundice.
It does not require treatment, and many doctors do not consider it a disease and consider it as a variant of the norm and an individual feature. Gilbert's syndrome occurs in 1-5% of the population, depending on the region. It is associated with a defect in the gene that is responsible for the production of a liver enzyme. Thanks to this enzyme, indirect bilirubin binds. In a third of Gilbert's syndrome carriers, the pathology does not manifest itself throughout life. It is often asymptomatic and is detected only by a blood test for bilirubin. However, more pronounced symptoms are also possible: pain in the right hypochondrium, metallic taste in the mouth, flatulence, vomiting, general weakness and fatigue, loss of appetite, insomnia. Symptoms are varied, and often patients with Gilbert's syndrome experience low mood, irritability, and anxiety.
There is usually no specific treatment for Gilbert's syndrome. The patient needs to limit the amount of fatty foods in the diet, adhere to a healthy lifestyle and visit a gastroenterologist - he is the one who diagnoses and treats this disease.
Why does physiological jaundice appear?
The jaundiced coloration of the baby’s skin is caused by bilirubin, a breakdown product of hemoglobin, which is contained in red blood cells. Normally, about 1% of all red blood cells die every day in a person, and the released bilirubin is immediately neutralized by special liver enzymes and excreted out by the excretory system.
Newborns usually have very high hemoglobin levels, which gradually decrease. That is, the process of death of red blood cells and release of bilirubin in a newborn is much more intense than in an adult. But the functions of the liver are not yet fully debugged, and there are simply not enough special liver enzymes to neutralize bilirubin. Therefore, bilirubin penetrates the skin cells and colors it yellow.
At the same time, there is no noticeable deterioration in well-being, changes in the size of internal organs, as is the case with pathological jaundice, as well as the color of feces and urine. The second reason for jaundice in a newborn is the loss of fluid by the child in the first days after birth and a small volume of colostrum.
Physiological jaundice of newborns lasts about three weeks. During this time, the baby’s liver improves its functions and acquires the ability to cope with the task of neutralizing bilirubin, which, by the way, is released less and less over time.
Sometimes the course of jaundice in newborns is longer, but this does not always indicate pathology - sometimes it is associated with breastfeeding. In this case, jaundice is also considered a physiological process and goes away on its own. But a prolonged course of jaundice necessarily requires examination by a pediatrician, and sometimes additional research.
Symptoms
Degree of jaundice
In addition to jaundice, the following symptoms are also present:
- the baby is lethargic and cries loudly;
- he has a decreased appetite;
- rest and sleep patterns are disrupted.
Signs of pathological jaundice
Changes in the functioning of the nervous system are observed. An increase in bilirubin levels is observed. On examination, the liver and spleen were enlarged.
Feces and urine show changes during examination. The newborn refuses to breastfeed. To stabilize the condition, they resort to treatment after diagnostic measures.
Diarrhea
Newborns rarely have diarrhea with jaundice. It can be observed at a later period after several months. This symptom indicates that the child’s liver function is impaired.
In the presence of diarrhea, infants are diagnosed with parenchymal jaundice. Diarrhea can be caused by an infection or a malfunction of the gastrointestinal tract. But the presence of diarrhea may have nothing to do with jaundice syndrome.
What it is?
This is a passing condition, the cause of which is an imperfect and poorly formed enzyme system in the child’s liver. When the fetus is still in the womb, bilirubin is automatically excreted through the placenta through the maternal bloodstream through the pregnant woman's liver.
But as soon as a child is born, the baby’s liver is not able to immediately remove substances in the required quantity on its own. Bilirubin in the blood begins to accumulate sharply and after a while it is several times higher than normal levels.
As a result, it provokes the appearance of jaundice, which persists in children born at a maximum of 10 days, and in premature infants for 2 weeks. With this syndrome, the baby’s general well-being does not deteriorate.
Watch in the video what Komarovsky says about newborn jaundice:
Jaundice syndrome
Doctors do not consider jaundice to be a disease. This is a syndrome that is a complex of specific symptoms. The main one is yellowness of the skin, sclera and mucous membranes. If this is physiological jaundice, it is not considered to be a pathology.
It’s just that immediately after birth, a kind of adaptation of the baby’s body to new and unusual conditions for the body occurs, under which the fetal hemoglobin is converted by a not yet fully formed enzyme system into normal.
In this case, no treatment is required. The baby is monitored by a pediatrician who must monitor bilirubin levels. This will prevent hyperbilirubinemia.
Signs of physiological jaundice
Why does jaundice occur?
Every minute, red blood cells are destroyed in the human body. At the same time, bilirubin is released into the blood. It's called free. In another way it is called indirect. This bilirubin turns out to be toxic to the body's cells. Free bilirubin then binds to special blood proteins and is transported to the liver.
In the liver, a number of further transformations occur with it with the participation of enzymes, which lead to the formation of bound bilirubin. It is also called direct. This bilirubin is part of bile, along with it it is transported to the intestines during the digestion of food.
In the intestine, under the action of a certain enzyme, bound bilirubin is converted back into free bilirubin. This free bilirubin is partially absorbed back into the blood from the intestines. Bilirubin compounds, which are part of bile, color urine and feces dark.
Normal bilirubin levels in a blood test from a vein are 8.5-20.5 µmol/l. This applies to older children and adults. An increase in bilirubin as a result of a number of reasons leads to a person developing jaundice.
If an adult develops jaundice, this indicates a problem in the body. But jaundice in newborns does not always indicate any disease.
Jaundice in adults
Jaundice is less common in adults than in children and can occur for many reasons, including:
- Hepatitis. This is an inflammatory disease of the liver, often caused by a virus. Hepatitis can be acute (completely curable) or chronic. Other causes of hepatitis: medications, drugs, alcohol, autoimmune diseases. Such liver damage eventually leads to jaundice.
- Blocked bile ducts. These thin tubes carry bile from the liver and gallbladder to the small intestine. Gallstones and tumors can block the ducts.
- Pancreatic cancer: It is the 10th most common cancer in men and the 9th most common cancer in women.
- Blood disorders that cause rapid breakdown of red blood cells.
Diagnosis and treatment of jaundice
A preliminary diagnosis can be made based on skin color, but we repeat that jaundice is not a disease, but a syndrome.
Therefore, all further diagnostics after the initial examination will be aimed at identifying the cause of the symptoms. If the skin or sclera turns yellow, the following tests must be taken:
- general blood analysis;
- general urine analysis;
- biochemical blood test, including a blood test for total bilirubin and direct bilirubin;
- urine test for total bilirubin and direct bilirubin;
- blood for antibodies to viral hepatitis.
The next stage is hardware diagnostics.
Ultrasound of the liver and biliary tract is often required. If prescribed by a doctor, an MRI or tomography may also be performed. Treatment is selected individually, depending on the causes of jaundice, the condition of the internal organs and the results of the studies. Jaundice has many types and manifestations, and its treatment is also varied.
Different specialists deal with different types of jaundice: therapists, infectious disease specialists, hematologists, oncologists. Which specialist will become the primary attending physician will become clear as a result of the examination. It is right to start the examination by taking laboratory tests and contacting a therapist.
Author:
Baktyshev Alexey Ilyich, General Practitioner (family doctor), Ultrasound Doctor, Chief Physician